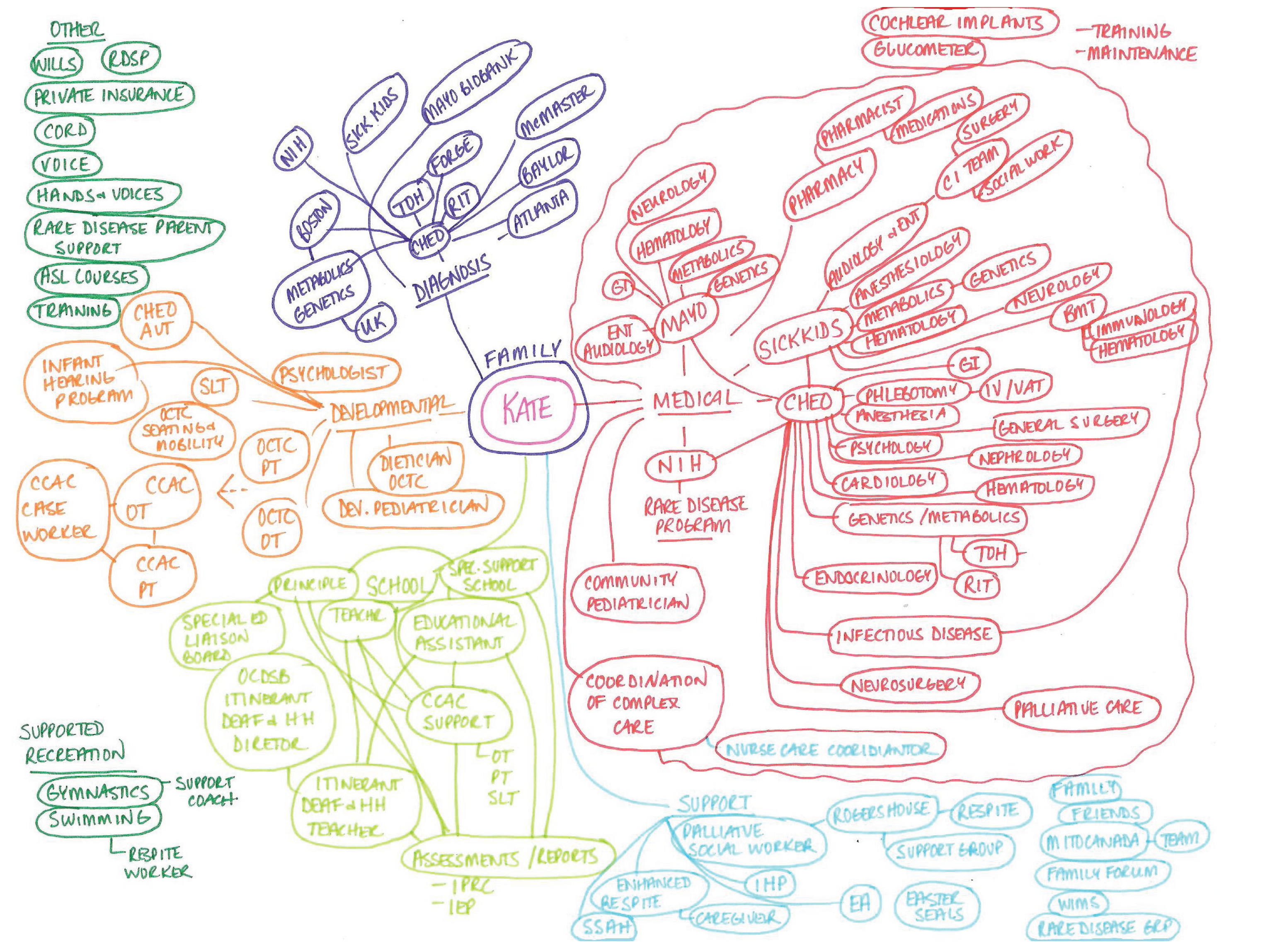
Children with medical complexity in Canada
 The burden of chronic disease is placing pressure on the Canadian health care system.
The burden of chronic disease is placing pressure on the Canadian health care system.
A small but important chronic disease population is children with medical complexity, defined as individuals with: high family-identified needs; complex chronic disease necessitating specialized care; functional disability; and high health care utilization.
These patients present a challenge to community providers who are expected to provide holistic care and manage complex issues, often with a paucity of services and supports.
Tammie Dewan MD, British Columbia Children’s Hospital, Vancouver BC and Eyal Cohen MD, The Hospital for Sick Children, University of Toronto, Paediatrics & Child Health December 2013
Alternative models of care may address the complex needs of this population. In addition, strategies can be implemented in community practices that may assist with the care of children with medical complexity such as collaborative care, engagement of key workers, focus on goal-directed care and use of care plans. The paediatric community should engage in health care reform discussions focused on chronic disease to ensure that the complex needs of these children are met.
Paediatric health care providers are caring for more patients with complex and chronic diseases, due, in part, to advances in intensive care and increased efficacy of treatments, which have resulted in improved survival rates. The term ‘children with special health care needs’ (CSHCN) describes a broad group of children who have medical, developmental or psychiatric conditions. CSHCN represent approximately 12% to 18% of the paediatric population in the United States and include such varied conditions as type 1 diabetes, attention-deficit hyperactivity disorder and cerebral palsy. One common feature of CSHCN is the requirement for additional health care services compared with the general population; however, there is substantial variation in the depth and breadth of their needs.
Governments and health care policy makers are trying to address the epidemic of chronic disease in Canada through primary care service reform, emphasis on patient-centred care, continuity of care and increased attention to the broader dimensions of health. Future changes in the health care system in Canada must account for provision of integrated care at both specialty institutions and community practices. Technology, such as teleconferencing and remote monitoring, will provide an unprecedented opportunity to improve the ability to care for patients with complex and chronic diseases in their home communities.
Although smaller in number than their adult counterparts, CMC should be included in these reforms and the development of new models of care. Some models and services that are designed for adults with chronic conditions may be transferred to the paediatric population. Successful comprehensive care models already exist in paediatrics, such as in the cystic fibrosis population, and could be applied to other groups, including CMC.
In addition to medical care, the models must address developmental and social needs, the health of caregivers and family members, and the need for a seamless future transition into adult care. The time is ripe for the paediatric community to collaborate in this health system transformation to ensure that children and youth are not left behind. A continued focus on integration across the continuum of care has the potential to enhance the quality of care delivery and improve the support provided for the families of these vulnerable patients.
Children with medical complexity in Canada, Tammie Dewan MD, Eyal Cohen MD. Paediatrics & Child Health Volume 18(10); 2013 Dec
Also see
National Center for Medical Home Implementation, Care Plans in American Academy of Pediatrics
OACRS Best Practice – Physiotherapy Intervention in School for Ambulatory School Age Children with Developmental Delay in Knowledge Exchange Network
New Model for Meeting the Needs of the Most Fragile Children in The Wall Street Journal
Road Map for Children With Special Health-Care Needs and Their Families in Navigate Life Texas
Nearly a Third of Early-Career Pediatricians Report Burnout in Medscape Medical News
Screening tools to identify developmental delay in healthy young children not beneficial, Canadian Task Force on Preventive Health Care updates guideline in EurekAlert! AAAS
Screening for developmental delay in children aged 1 to 4 years (2016) in Canadian Task Force on Preventive Health Care. The Public Health Agency of Canada and The University of Calgary.