Device is an easier option to correct chest deformity

Dr. Robert Obermeyer of Children’s Hospital of The King’s Daughters in Norfolk shows Austin Hinton and his mother, Tina Hinton, how to operate Austin’s new “vacuum bell” on Wednesday, Nov. 21, 2012. The vacuum bell is an apparatus used to treat a chest deformity called “pectus excavatum,” in which the chest is concave. Amanda Lucier, The Virginian-Pilot
By Elizabeth Simpson, The Virginian-Pilot November 22, 2012
If you can visualize the suction cup an auto shop uses to pop out a dent in a car door, you can imagine the device 13-year-old Austin Hinton was outfitted with Wednesday at a local children’s hospital.
Hinton has what’s called “pectus excavatum,” a condition in which the breastbone bows inward instead of outward. It’s the most common chest deformity, and Children’s Hospital of The King’s Daughters has become the go-to facility for correcting it.
That’s largely due to a minimally invasive procedure that surgeon Donald Nuss developed at CHKD in the late 1980s. Since then, more than 1,700 children and young adults have come here for “the Nuss procedure,” which involves small incisions on either side of the chest, and a steel bar inserted under the sternum to push it out over a period of about two years.
Now the hospital is trying a device called a vacuum bell that doesn’t require surgery at all and has been growing in use in European countries the past five years.
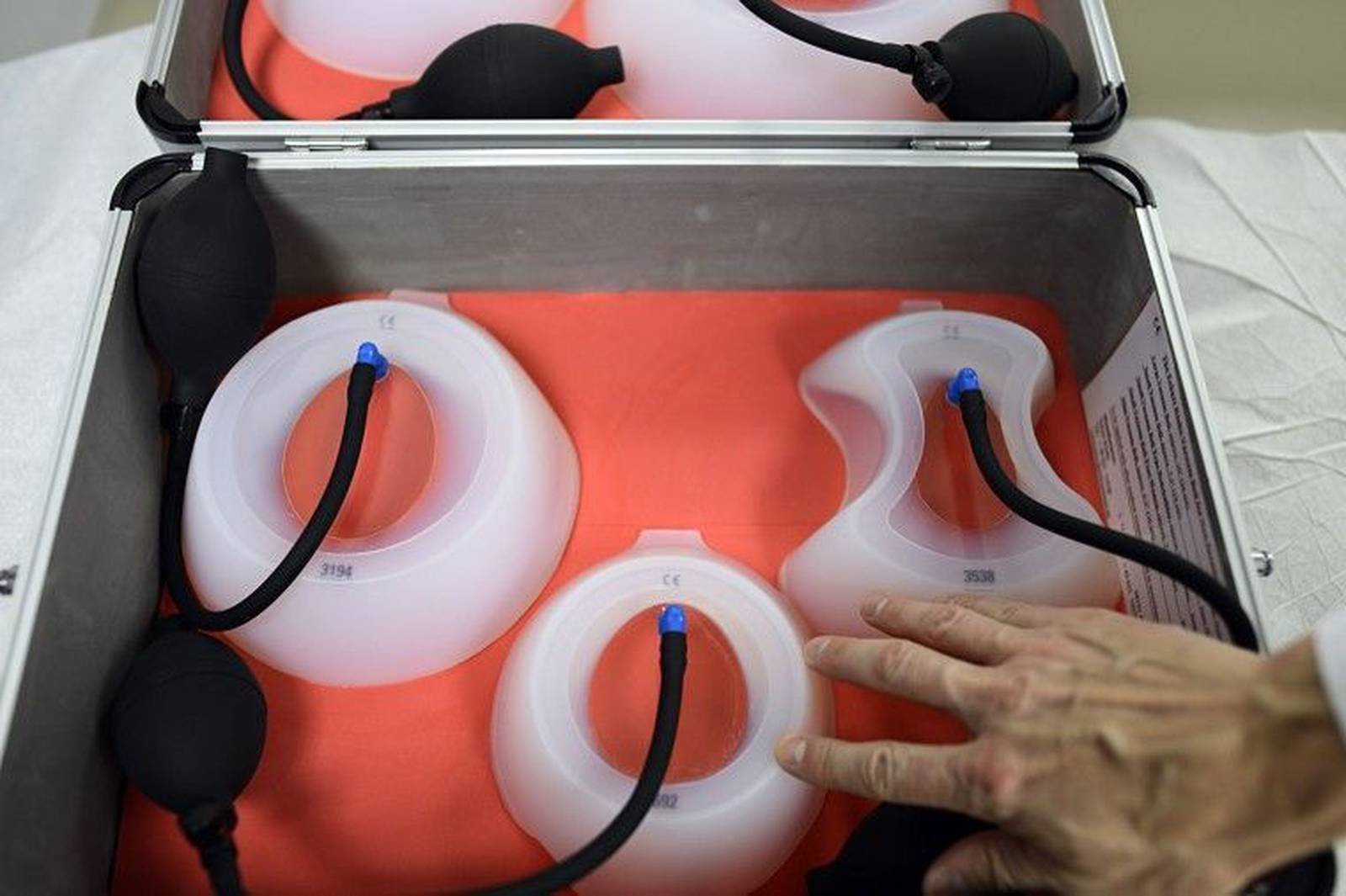
Dr. Robert Obermeyer of Children’s Hospital of The King’s Daughters in Norfolk shows a case of “vacuum bells” on Wednesday, Nov. 21, 2012. A vacuum bell is an apparatus used to treat a chest deformity called “pectus excavatum,” in which the chest is concave. Amanda Lucier, The Virginian-Pilot
Basically, it’s a suction cup that’s placed on the outside of the chest wall. The patient uses a hand pump for 30 minutes to a couple of hours twice a day to create pressure within the device that slowly lifts the chest wall over a period of about a year.
The device is still in the experimental phase in this country, but CHKD received clearance to use it after a German developer submitted paperwork to the Food and Drug Administration qualifying the vacuum bell as a Class 1 medical device.
Those devices are noninvasive and present such a low level of risk that they don’t require the same rigorous testing that higher classes of devices, such as pacemakers and joint replacements, must provide for FDA approval.
It sounds too low-tech to be true, and chatter on message boards of support groups of people with the chest deformity range from the skeptical to those wanting to try it.
The vacuum bell CHKD is using was developed in Germany by engineer Eckart Klobe, who used it to correct the dip in his own chest.
He’s worked closely with a surgeon in Switzerland, Dr. Frank-Martin Haecker, who has used the device with patients, and tracked its effects. A study he published in the Journal of Clinical and Analytical Medicine last year of 93 patients found it improved the condition in a majority of cases, and in 10 percent brought the chest wall into the normal range.
Haecker’s study noted, though, that there are currently no long-term data of the device’s use – he followed patients for five years – and the numbers in studies so far have been small.
Complications include bruising under the skin, and the device is not recommended for people with skeletal, bleeding or heart disorders. It’s not known yet how long the improvements will last.
Local pediatric surgeon Robert Obermeyer felt it was an important option to study and include in CHKD’s program. The hospital performs more surgeries to correct the chest wall deformity than any hospital in the country. Obermeyer flew to Switzerland during the summer to observe Haecker’s consultations with patients, and he also visited Klobe’s business in Germany.
Obermeyer believes this technique will be an option for mild to moderate cases that don’t qualify for surgery. It could also be used as a first option in more severe cases to see if enough progress can be made that surgery wouldn’t be necessary.
If the long-term results prove positive, it could save thousands of dollars in surgery costs, along with the pain and inconvenience of hospital stays.
In some cases, a sunken breastbone is noticed shortly after birth; in others, it first becomes apparent during puberty. Sometimes it’s only a cosmetic concern that doesn’t require correcting.
But more severe cases of the condition, which is caused by too much connective tissue between the ribs and the breastbone, can interfere with breathing and heart function.
It’s estimated that 1 in 1,000 children have some form of the condition.
Tina Hinton said her son Austin started noticing the dip in his chest when he was about 12. He had a growth spurt during the past year that worsened the condition. They traveled from their home in Heathsville on the Northern Neck to CHKD for consultation.
Obermeyer suggested the vacuum bell. Although insurance doesn’t cover it yet in the United States, Hinton said she and her husband decided it was the best method to try. Hinton said they expect to pay about $1,000 for the device.
“It was a no-brainer, since it didn’t involve surgery,” Hinton said. “I thought it was a fascinating concept.”
She works in the dental field and thought it was similar to the idea of expanders widening the palate to produce a better jaw alignment.
Austin will need to use the air pressure pump every day, for 30 minutes to a couple of hours, for a year to 18 months for the best results. Obermeyer said some teens think the more they use it, the faster it will work, but that’s not necessarily the case: “You will not lift your chest; you’ll stretch your skin.”
Austin is the second patient CHKD has outfitted with the device. A 15-year-old boy from Birmingham, Ala., received one on Nov. 14.
In a phone interview, the mother of the 15-year-old said her son didn’t want his name used because he had been made fun of in the locker room for having the condition. She said he was going to have the Nuss procedure in Birmingham, but the surgeon advised waiting a year.
In the meantime, she read about the vacuum bell on the Internet and discovered CHKD was offering the method.
Her son has been using the vacuum bell for 20 minutes a day and will build up to longer periods. She said they can see that his chest is less concave after use, and they’re hoping daily use of the device will lead to permanent results.
If not, there’s still the option of surgery.
Obermeyer said he’ll be examining the patients every three months and entering results in a database of 3,000 patients with the condition, which is the largest such database in the country.
If the results are positive, it could lead to fewer surgeries for the condition, said Obermeyer:
“It’s important for us, of all people, to give patients options, since we take care of more people with this condition than anywhere in the U.S.”
| Elizabeth Simpson | 1-757-446-2635 | elizabeth.simpson@pilotonline.com |
![]() Source The Virginian-Pilot
Source The Virginian-Pilot
| Children’s Hospital of The King’s Daughters offers the Vacuum Bell as a non-invasive approach to correcting pectus excavatum. Dr. Robert Obermeyer directs CHKD’s usage of the Vacuum Bell. Visit CHKD.org to learn more. Youtube Feb 13, 2015 |
| References |
The Vacuum Bell for Treatment of Pectus Excavatum: An Effective Tool for Conservative Therapy, Haecker FM. J Clin Anal Med. 2011;2(1):1-4. DOI: 10.4328/JCAM.314
| Further reading |
The vacuum chest wall lifter: an innovative, nonsurgical addition to the management of pectus excavatum, Schier F, Bahr M, Klobe E. J Pediatr Surg. 2005 Mar;40(3):496-500. doi: 10.1016/j.jpedsurg.2004.11.033.
The vacuum bell for treatment of pectus excavatum: an alternative to surgical correction? Haecker FM, Mayr J. Eur J Cardiothorac Surg. 2006 Apr;29(4):557-61. doi: 10.1016/j.ejcts.2006.01.025. Epub 2006 Feb 13. Full text, PDF
The vacuum bell for conservative treatment of pectus excavatum: the Basle experience, Haecker FM. Pediatr Surg Int. 2011 Jun;27(6):623-7. doi: 10.1007/s00383-010-2843-7.
Vacuum bell therapy, Haecker FM, Sesia S. Ann Cardiothorac Surg. 2016 Sep;5(5):440-449. doi: 10.21037/acs.2016.06.06. Full text, PDF
Incorporating vacuum bell therapy into pectus excavatum treatment, Obermeyer RJ. J Vis Surg. 2016 May 18;2:99. doi: 10.21037/jovs.2016.05.01. Full text, PDF
The Vacuum Bell device as a sternal lifter: An immediate effect even with a short time use, Togoro SY, Tedde ML, Eisinger RS, Okumura EM, de Campos JRM, Pêgo-Fernandes PM. J Pediatr Surg. 2018 Mar;53(3):406-410. doi: 10.1016/j.jpedsurg.2017.04.016. Epub 2017 May 1.
Nonoperative management of pectus excavatum with vacuum bell therapy: A single center study, Obermeyer RJ, Cohen NS, Kelly RE Jr, Ann Kuhn M, Frantz FW, McGuire MM, Paulson JF. J Pediatr Surg. 2018 Jun;53(6):1221-1225. doi: 10.1016/j.jpedsurg.2018.02.088. Epub 2018 Mar 8.
Broad Pectus Excavatum Treatment: Long Term Results Of A Brazilian Technique, Haje DP, Haje SA, Volpon JB, da Silva ACO, Lima LFB, Huang W. Acta Ortop Bras. 2021 Jul-Aug;29(4):197-202. doi: 10.1590/1413-785220212904243419. Full text, PDF
Also see
First patients in US receive non-surgical device of sunken chest syndrome Science Daily
Surgeons demonstrate new minimally invasive technique to correct chest deformity Science Daily
Cialis Daily er et nyt mærke af Cialis, som kan fås på apoteket uden recept. Det er den samme medicin som tadalafil, eller generisk Cialis, som vores online apotek også leverer. Køb Viagra uden recept (tadalafil) er medicinsk identisk med det tilsvarende mærke - se ofte stillede spørgsmål om generisk medicin.