Battle of Achilles II: How the debate is informing clinical practice
Four years later, the ongoing discussion of the relative merits of surgical and nonsurgical management of Achilles tendon rupture is starting to affect practice patterns – even in the US.

Sara Mearns, New York City Ballerina. Photography by Erin Kestenbaum.
By Cary Groner, Lower Extremity Review November 2015
When LER first reported on research concluding that nonsurgical and surgical treatment of Achilles tendon rupture yielded similar outcomes,[1] the issue had become so contentious that a shouting match erupted at the 2011 meeting of the American Academy of Orthopaedic Surgeons (AAOS). Now, four years later, clinicians on both sides still defend their positions even as they’ve begun to inch toward common ground.
The goal of Achilles rupture management, regardless of approach, is homogenous healing, regeneration, and functional restoration.[2] To achieve this, clinicians must avoid complications such as rerupture and infection. Unfortunately, these aims can be mutually contradictory; studies suggest that surgery is associated with lower rerupture rates than nonoperative management but a higher risk of infection. Nonsurgical approaches pose their own challenges, including patient compliance with rehabilitation protocols that can be frustrating and prolonged.[2]

Sara Mearns, New York City Ballerina. Photography by Erin Kestenbaum
| Incidence and demographics |
Study results have begun to affect practice patterns regardless, particularly in Europe. For example, a recent study in the American Journal of Sports Medicine (AJSM) reported that in Sweden between 2001 and 2012, surgical treatment declined from 43% to 28% of cases in men, and from 34% to 22% in women.[3]
Varying increases in incidence of Achilles rupture have been observed worldwide. Over 33 years, incidence in one Finnish city rose dramatically from 2.1 to 21.5 per 100,000 person-years in all age groups.[4] By contrast, a recent study in Denmark found that, though there was just a slight incidence increase from 1994 to 2013, the most significant rise occurred in those older than 50 years; in those aged 31 to 50 years, there was no significant change, and in those aged 18 to 30 years, there was a decrease in ruptures.[5]
“I believe the incidence increase is due to older people remaining active in sports,” said one of the study’s authors, Kristoffer Barfod, MD, PhD, who practices at Hvidovre University Hospital in Copenhagen.
The bump in cases isn’t just a European phenomenon.
“We’re seeing older people with very high activity levels, and I think that’s one reason for the increased rates,” agreed Lowell Weil Jr, DPM, who is chief executive officer of Weil Foot & Ankle USA, in Des Plaines, IL. “As we get older we become less flexible, and injuries that might have been a pull or a partial tear in a younger person become complete ruptures because the tissue isn’t as tensile.”
David Richardson, MD, an orthopedist at the University of Tennessee-Campbell Clinic in Memphis, said the Achilles ruptures he sees are often in patients involved in high-intensity sports protocols or exercise regimens.
“Instead of walking for thirty minutes, they’re doing intense routines for six minutes, and I think that overloads the tendon,” Richardson said.
According to Jonathan Chang, MD, a clinical associate professor of orthopedics at the University of Southern California in Los Angeles, increasing incidence in the US might be attributable to the opposite of increased activity in older people—that is, sedentary behavior and the obesity that comes with it.
“The more weight you carry, the more stress you put on the tendon,” Chang said.
The trend may apply to the chronic problems that often precede acute tears, as well.
“I’m seeing a huge increase in Achilles tendinitis,” said Stuart Miller, MD, who practices in the Department of Orthopedic Surgery at Union Memorial Hospital in Baltimore, MD. “Most Achilles ruptures arise out of chronic conditions. Some of these people just exercise once or twice a week—say, go out and play basketball on the weekend. Their gastrocnemius muscles just get tighter and tighter, and pull too hard on the Achilles.”
| To cut or not to cut |
The uptick in cases, and the older patients sometimes affected, may influence clinicians’ decisions about approach to treatment, but not always in predictable ways. Invariably, the discussion circles back to whether surgery is the best option for any given patient.
The Canadian meta-analysis that provoked the AAOS skirmish found if patients had functional rehab including early range-of-motion (ROM) exercises, rerupture rates were equal for surgical and nonsurgical patients.[6] Without early ROM therapy, surgery had an 8.8% lower rerupture risk but a 15.8% higher risk of other complications, both statistically significant differences. Surgical patients returned to work significantly (19 days) sooner, but the treatments were equivalent in terms of strength and functional outcomes. (The authors could not be reached for comment.) That study followed a 2010 study, also from Canada, that also found outcomes to be similar between groups and recommended functional rehab and nonsurgical treatment.[7]
But not all research has reached similar conclusions. For example, a 2008 paper compared risk of complication other than rerupture and reported a rate of 21% for surgical treatment versus 36% for nonsurgical therapy (many of the complications in the nonoperative group were minor skin problems related to brace wear). As in most studies, moreover, return to work was significantly faster with surgery—59 days versus 108 days for those treated nonoperatively.[8]
Another issue is that, although research consistently finds higher rerupture rates in nonsurgically treated patients than their surgical counterparts, the between-group differences are often not statistically significant. Even so, the papers usually shed light on related matters.
For example, in a 2010 article in AJSM,[9] Scandinavian researchers reported rerupture rates of 4% in the surgical group and 12% in the nonsurgical group—not a statistically significant difference, but one the authors said might be considered clinically important. Although muscle function was better in the surgical patients at six months, the two groups were about the same by 12 months.
In a 2011 paper in the Journal of Bone and Joint Surgery,[10] researchers reported rerupture in 5% of operative patients and in 10% of those in the nonoperative group, a nonsignificant difference. The between-limb difference in plantar flexion peak torque was significantly smaller in those treated surgically, as well, though the disparity disappeared a year out from treatment.
The authors of a 2012 systematic review reported that surgical repair was associated with a 3.6% rerupture rate, versus 8.8% for nonsurgical treatment—a statistically significant difference in this case.[11] Surgically treated patients had a higher incidence of deep infections, scarring, and sural nerve disturbances, however.
Then, in 2013, another Scandinavian study reported that in 100 patients, there were no reruptures in the surgical group (n = 49) but five in the nonsurgical group, a finding that trended toward statistical significance. Operative treatment was not deemed superior in other variables, however, including physical function and quality of life.[12]
Finally, a 2014 meta-analysis found that rerupture rates were 3.6% and 8.8% for patients treated with open surgery and nonsurgically (odds ratio .425 favoring surgery), respectively, though other complications such as infections and scarring were higher in surgical patients.[13]
| Clinical experience and technique |
US surgeons have questioned some of these findings based on their own experience.
“The Canadian study by Soroceanu [6] showed a fairly high incidence of skin problems with an open Achilles tendon repair, something like fifteen percent,” Stuart Miller said. “I’d never seen anything like that, so I went through our records of more than two hundred acute Achilles ruptures over twenty years, and found a two or three percent incidence of skin problems.”
Miller, who was the moderator at the 2011 AAOS meeting when tempers flared, acknowledges a trend toward nonoperative treatment, but still has qualms.
“I think it slows down recovery,” he said. “My athletes and very active patients definitely get open repair. The patient is just more likely to stretch out a tendon that’s healed by scar formation and fibrosis and reformation. For the first year or two, that’s not going to be as strong as a thick suture holding everything together.”
Miller emphasized, moreover, that in his 21 years of practice only one of his patients has had a postsurgical infection, so he remains skeptical about some of the numbers reported in the literature. He’s not alone.
“Mark Twain said there are lies, damned lies, and statistics,” Richardson said. “Sometimes it’s hard to get numbers such as rerupture rates to reach statistical significance. That’s part of why some of us don’t abandon surgery — we see in our practices that patients get stronger faster that way. Operative risks are much lower than they used to be, too, because our approaches have improved.”
Chang concurred.
“Maybe it boils down to technique, but I’ve not had any problems with skin healing, and I’ve never had an infection,” he added. He continues to use an open approach with a Krakow suturing technique, which he feels offers the strongest fixation.
“In my practice I have a zero rate of rerupture,” he continued. “That was one of my objections to the Scandinavian studies; they did a modified Kessler stitch, and you have to immobilize longer if you don’t trust your repair.”
Other surgeons have opted for less invasive approaches, often involving Achilles repair devices such as the Percutaneous Achilles Repair System (PARS). Lowell Weil uses PARS, as does Richardson.
“It allows me to put a suture inside the Achilles sheath and lock it,” Richardson said. “It’s a small, two-centimeter incision, and because of that there’s a very low complication rate.”
Stuart Miller prefers a core-weaving technique developed by his colleague, Greg Guyton, MD.
“It’s like a Krakow, but we do a cross stitch and bury the suture within the tendon most of the way, which theoretically lets the tendon glide more easily,” he said. “The incision heals side-to-side, which I think puts less strain on the tissues. It also lets me go up a little higher to get a good bite of tendon.”
| Patient profiles |
All that said, clinicians told LER that they’re getting more comfortable with the idea of nonsurgical repair. Often the decision has to do with patient profile.
“People in sports medicine still have a bias that, for an elite athlete, a nonoperative treatment is not likely to be as good,” Chang said. “My patient population is tilted toward sports people, and they recognize that there is triple the risk of rerupture nonoperatively, so eighty percent say they want surgery.”
Chang added that he’s more open to nonoperative approaches than he used to be, however. Recently, in fact, he saw a patient with a chronic Achilles rupture who had never received any treatment at all.
“She came to see me two months after the injury, during which she’d basically gotten around by limping,” he said. “Even so, she’d reconnected her Achilles tendon without any immobilization. That’s evidence that nonoperative approaches can work.”
Chang also believes that patients older than 40 years, who are no longer elite athletes if they ever were, have a better chance of successful nonoperative treatment.
“I now see this more as a continuum,” he said. “If you tear your Achilles when you’re twenty, it’s a much more devastating injury than if you’re eighty because of your activity level. The average sedentary person will have a longer recovery, but by two months out they have enough connection that they can start to push off a little bit, and as long as they see ongoing improvement they do well.”
Stuart Miller also said that he’s more open to nonoperative repair. He’s treated only four cases nonoperatively in the past 10 years, but that’s twice the number he did in the decade before that.
“It depends on the individual,” he explained. “One of those patients was an older doctor, in his late eighties, who’d read the research and decided he wanted a nonoperative approach. He did fine.”
Miller believes that other arguments for a nonsurgical approach may include medical problems that may delay healing, including smoking and obesity.
Kristoffer Barfod, in Copenhagen, has a different take on patient profiling.
“I’m starting to think we should reverse the approach we’ve used before,” he said. “My experience is that young, active people who can follow the nonoperative rehabilitation regimen heal very fast. On the other hand, some older people don’t accept that they have an injury because there isn’t much pain, so they keep walking and pull the tendon apart. If you operate, you secure the tendon and immobilize them so they can heal.”
Lowell Weil agrees.
“I think there are advantages to surgery in older people, because they’re the ones least able to handle long periods in a cast,” he said. “If we can get them out of the immobilizing device faster by operating, then I go that route.”
| All in the timing |
Timing also affects treatment decisions, according to Barfod.
“If you wait too long, you miss the time period for doing a nonsurgical treatment,” he said. “You get an elongation of the tendon callus, then it shrinks. I believe it’s crucial [in nonoperative treatment] to keep the foot in maximum plantar flexion for two weeks after injury in order to get a tendon callus of the correct length. If you start treatment too late you won’t get that, and then you should probably choose a surgical approach. In our institution, if you come in later than four days, you get surgery.”
Other surgeons have varying opinions about timing.
For David Richardson, if patients present with a chronic injury more than four weeks old, they’re likely to get an open surgery rather than the PARS approach.
“The tendon edges tend to be retracted, scarred in, and not very mobile by then,” he said. “It depends on what sort of deficit they have when they come in, however. If they’re doing reasonably well, I might just recommend rehab alone.”
Though physicians report anecdotally that surgical cases proceed more quickly than nonsurgical cases, they allow that long-term outcomes may not differ significantly.
Jonathan Chang will consider surgery up to three or four weeks out if the patient has kept weight off the injured limb, say, by using crutches.
“My general rule is that if it’s more than three weeks, it’s probably too late, because by then the ends of the tendon are like the ends of a mop,” he said. “It’s difficult to put it back together adequately. My optimal time is generally seven to ten days after injury; I think most people prefer not to operate right afterward because you run into bleeding and you don’t know the viability of the tissue yet.”
Surgeons said they increasingly rely on ultrasound to assess tendon status. A 2011 article in ISRN Orthopedics provided a roadmap of seven classes of sonographic findings and the implications they held for treatment decisions,[2] though it isn’t clear how widely they’ve caught on in the clinical community.
| Rehabilitation |
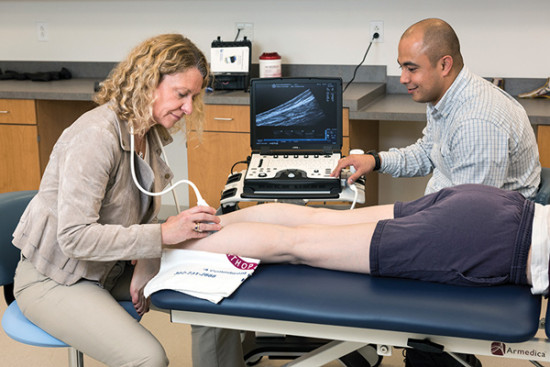
Researchers at the University of Delaware in Newark are using a new ultrasound-based technique to better understand the effects of rehabilitation on the Achilles tendon, which could help optimize rehab protocols to improve long-term function. Read the Shear-wave elastography could help optimize Achilles rehab article in Lower Extremity Review
Whether patients are treated surgically or nonsurgically, they still face rehabilitation, and, though physicians report anecdotally that surgical cases typically proceed more quickly, they also allow that long-term outcomes may show little difference.
“Early on, a surgical repair does better, but somewhere between eighteen and twenty-four months they equalize,” Stuart Miller said.
Published studies usually address one of three conditions: postsurgical therapy; therapy after operative versus nonoperative treatment; or nonoperative rehabilitation alone.
In the first category, a 2015 randomized controlled trial (RCT) in Australia compared an accelerated mobilization rehab protocol with standard (immobilization) care.[14] Patients in the accelerated treatment group (n = 25) had less tendon lengthening and a quicker return to running than those in the standard group (n = 26), but similar results in the Achilles tendon Total Rupture Score (ATRS). The authors concluded that immobilization may prolong recovery.
A 2015 meta-analysis looked at 10 trials comprising 570 patients; some received early functional postoperative ankle motion and weightbearing (bracing group), whereas others had ankle immobilization with a nonweightbearing rigid cast (cast group).[15] In the bracing group, patients returned to preinjury activity levels faster and reported better satisfaction; there was no difference in complication rates.
In the second category—therapy after operative or nonoperative treatment—researchers in the Netherlands conducted a meta-analysis of rerupture rate and other variables in patients who began weightbearing within four weeks after surgery versus nonoperative care patients with similar weightbearing regimens.[16] Rerupture rates were 4% and 12% in the surgical and nonsurgical patients, respectively; a secondary analysis of patients who began weightbearing later than four weeks found rerupture rates were slightly higher in the surgical patients (6%) but lower in the nonsurgical group (10%). Neither between-group difference was statistically significant.
In the third category—rehab regimens in nonoperative patients—Danish researchers conducted an RCT comparing full weightbearing from day one to nonweightbearing for six weeks.[17 ]After a year, those in the weightbearing group had a better ATRS score, though rerupture rate was 9% in both groups, and both retained functional deficits in the injured limb. In a later analysis of biomechanical data from the same study, the researchers reported increased stiffness of the plantar flexor muscle-tendon complex in the nonweightbearing group at one year.[18]
“We concluded that weightbearing improved quality of life and did not have detrimental effects on functional outcomes,” said Kristoffer Barfod, who was the lead author of both papers.
Other clinicians described their preferred rehabilitation regimens to LER. David Richardson keeps his patients nonweightbearing for two weeks, than has them bear weight as tolerated in a boot with a triple (3″) heel lift. After the initial two weeks in the boot, patients can remove it and work on general ROM, stopping if they feel pain or reach neutral (90° of ankle dorsiflexion).
“Each two weeks they remove one of the one-inch heel lifts, and they come out of their boot at about eight weeks,” he said. “That’s when they begin more aggressive physical therapy, but I keep them in a brace with a small heel lift until twelve weeks.”
Lowell Weil leaves his postoperative patients in a nonweightbearing cast for two weeks, then switches them to a removable boot with slight equinus (plantar flexion). “I start them with gentle physical therapy at two weeks—range of motion and muscle stimulation—then at twenty-eight days postop I let them fully weightbear with a small heel lift in their walking boot,” he said. “At six weeks they return to gym shoes.”
Practitioners should get patients moving as soon as safely possible, Stuart Miller said.
“It provides a better environment for tendon healing and makes for a stronger tendon later,” he said. “After surgery, I only keep them immobilized for the first week, then I put them in a boot. They can come out of that to plantar flex–dorsiflex three times a day so they don’t scar down. Then, when we start formal physical therapy at six weeks, they already have almost all their motion back.”
Miller admitted that he handles nonsurgical cases more delicately.
“We’re hesitant to stretch them too quickly,” he said. “Some people start moving them gently at two or three weeks, others wait a month. I don’t know what that magic number is.”
Jonathan Chang added that, for him, the quality of initial treatment is the most important factor in rehabilitation.
“If you’ve done a solid repair you can feel comfortable pushing them a little bit because the repair itself isn’t going to be the limiting factor,” he said.
These variations in rehabilitation protocols indicate the degree to which clinicians rely on experience and observation to produce individualized treatment plans for their patients. But there are innovations on the horizon (see sidebar) that may soon provide more objective measures.
| Cary Groner is a freelance writer in the San Francisco Bay Area |
Source Lower Extremity Review
| References |
- Battles of Achilles: The operative vs nonoperative treatment debate, Groner C. LER 2011;3(5):14-21.
- Ultrasonographic classification of achilles tendon ruptures as a rationale for individual treatment selection, Amlang MH, Zwipp H, Friedrich A, Peaden A, Bunk A, Rammelt S. ISRN Orthop. 2011 Oct 24;2011:869703. doi: 10.5402/2011/869703. Full text
- Acute achilles tendon ruptures: incidence of injury and surgery in Sweden between 2001 and 2012, Huttunen TT, Kannus P, Rolf C, Felländer-Tsai L, Mattila VM. Am J Sports Med. 2014 Oct;42(10):2419-23. doi: 10.1177/0363546514540599. Epub 2014 Jul 23.
- Epidemiology of Achilles tendon ruptures: increasing incidence over a 33-year period, Lantto I, Heikkinen J, Flinkkilä T, Ohtonen P, Leppilahti J. Scand J Med Sci Sports. 2015 Feb;25(1):e133-8. doi: 10.1111/sms.12253. Epub 2014 May 23.
- Increasing incidence of acute Achilles tendon rupture and a noticeable decline in surgical treatment from 1994 to 2013. A nationwide registry study of 33,160 patients, Ganestam A, Kallemose T, Troelsen A, Barfod KW. Knee Surg Sports Traumatol Arthrosc. 2016 Dec;24(12):3730-3737. doi: 10.1007/s00167-015-3544-5. Epub 2015 Feb 20.
- Surgical versus nonsurgical treatment of acute Achilles tendon rupture: a meta-analysis of randomized trials, Soroceanu A, Sidhwa F, Aarabi S, Kaufman A, Glazebrook M. J Bone Joint Surg Am. 2012 Dec 5;94(23):2136-43. doi: 10.2106/JBJS.K.00917. Full text
- Operative versus nonoperative treatment of acute Achilles tendon ruptures: a multicenter randomized trial using accelerated functional rehabilitation, Willits K, Amendola A, Bryant D, Mohtadi NG, Giffin JR, Fowler P, Kean CO, Kirkley A. J Bone Joint Surg Am. 2010 Dec 1;92(17):2767-75. doi: 10.2106/JBJS.I.01401. Epub 2010 Oct 29.
- Acute Achilles tendon rupture: minimally invasive surgery versus nonoperative treatment with immediate full weightbearing–a randomized controlled trial, Metz R, Verleisdonk EJ, van der Heijden GJ, Clevers GJ, Hammacher ER, Verhofstad MH, van der Werken C. Am J Sports Med. 2008 Sep;36(9):1688-94. doi: 10.1177/0363546508319312. Epub 2008 Jul 21.
- Acute achilles tendon rupture: a randomized, controlled study comparing surgical and nonsurgical treatments using validated outcome measures, Nilsson-Helander K, Silbernagel KG, Thomeé R, Faxén E, Olsson N, Eriksson BI, Karlsson J. Am J Sports Med. 2010 Nov;38(11):2186-93. doi: 10.1177/0363546510376052. Epub 2010 Aug 27.
- Operative versus non-operative treatment of acute rupture of tendo Achillis: a prospective randomised evaluation of functional outcome, Keating JF, Will EM. J Bone Joint Surg Br. 2011 Aug;93(8):1071-8. doi: 10.1302/0301-620X.93B8.25998. Full text.
- Operative versus nonoperative management of acute Achilles tendon ruptures: a quantitative systematic review of randomized controlled trials, Wilkins R, Bisson LJ. Am J Sports Med. 2012 Sep;40(9):2154-60. doi: 10.1177/0363546512453293. Epub 2012 Jul 16.
- Stable surgical repair with accelerated rehabilitation versus nonsurgical treatment for acute Achilles tendon ruptures: a randomized controlled study, Olsson N, Silbernagel KG, Eriksson BI, Sansone M, Brorsson A, Nilsson-Helander K, Karlsson J. Am J Sports Med. 2013 Dec;41(12):2867-76. doi: 10.1177/0363546513503282. Epub 2013 Sep 6. PDF
- Outcomes of open surgery versus nonoperative management of acute achilles tendon rupture, Amendola A. Clin J Sport Med. 2014 Jan;24(1):90-1. doi: 10.1097/JSM.0000000000000064.
- Randomized controlled trial of accelerated rehabilitation versus standard protocol following surgical repair of ruptured Achilles tendon, Porter MD, Shadbolt B. ANZ J Surg. 2015 May;85(5):373-7. doi: 10.1111/ans.12910. Epub 2014 Nov 4.
- Early functional rehabilitation or cast immobilisation for the postoperative management of acute Achilles tendon rupture? A systematic review and meta-analysis of randomised controlled trials, McCormack R, Bovard J. Br J Sports Med. 2015 Oct;49(20):1329-35. doi: 10.1136/bjsports-2015-094935. Epub 2015 Aug 17.
- Rerupture rate after early weightbearing in operative versus conservative treatment of Achilles tendon ruptures: a meta-analysis, van der Eng DM, Schepers T, Goslings JC, Schep NW. J Foot Ankle Surg. 2013 Sep-Oct;52(5):622-8. doi: 10.1053/j.jfas.2013.03.027. Epub 2013 May 7.
- Nonoperative dynamic treatment of acute achilles tendon rupture: the influence of early weight-bearing on clinical outcome: a blinded, randomized controlled trial, Barfod KW, Bencke J, Lauridsen HB, Ban I, Ebskov L, Troelsen A. J Bone Joint Surg Am. 2014 Sep 17;96(18):1497-503. doi: 10.2106/JBJS.M.01273.
- Nonoperative, dynamic treatment of acute achilles tendon rupture: influence of early weightbearing on biomechanical properties of the plantar flexor muscle-tendon complex-a blinded, randomized, controlled trial, Barfod KW, Bencke J, Lauridsen HB, Dippmann C, Ebskov L, Troelsen A. J Foot Ankle Surg. 2015 Mar-Apr;54(2):220-6. doi: 10.1053/j.jfas.2014.11.018. Epub 2015 Jan 21.
Also see
BATTLES OF ACHILLES: The operative vs nonoperative treatment debate Lower Extremity Review
Shear-wave elastography could help optimize Achilles rehab Lower Extremity Review
YouTube ‘epic fail’ star-turned-researcher finds Achilles surprisingly adaptable Brigham Young University
