Pectus carinatum: The other deformational molding orthosis
There are two predominant types of congenital chest wall deformities. Pectus excavatum, also described as “cave chest” or “funnel chest,” is the most common with a prevalence of roughly 1 in 400 children. The sunken chest of pectus excavatum is five times more common than the opposite presentation of pectus carinatum or “pigeon chest.”
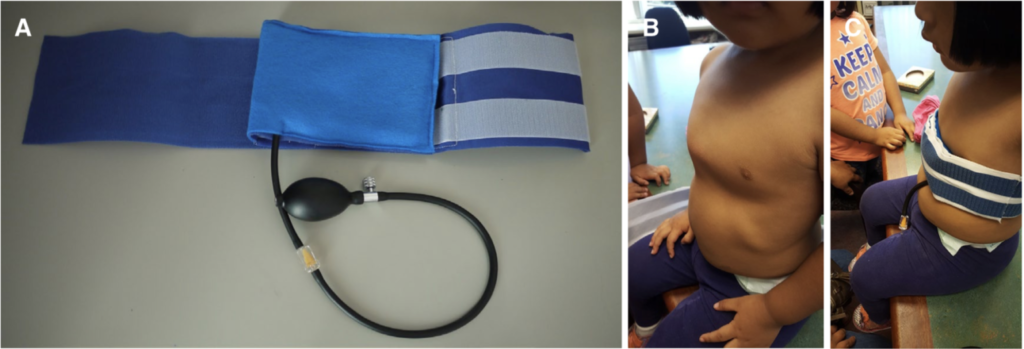
Figure 1. (A) A picture of the balloon brace; (B) a patient with symmetric pectus carinatum; (C) a patient wearing the brace. Ewbank et al. 2018.
By Phil Stevens MEd CPO FAAOP, THE O&P EDGE August 2020
Present in childhood, but progressively more noticeable during the rapid growth years of puberty, pectus carinatum may be the more noticeable of the two presentations because the associated prominence of the protruding chest wall can’t be hidden by clothing.
Historically, pectus carinatum was managed surgically. However, in the early 1990s, reports of conservative management using orthoses began to emerge. Between 1990 and 2000, three such articles were published, including two case studies and one preliminary report. Between 2000 and 2010, the frequency of such articles more than tripled, with 11 publications on the orthotic management of pectus carinatum. Since 2010, the prevalence has tripled again with 33 additional publications.
The broad acceptance of conservative management of pectus carinatum was reflected in the 2012 guidelines of the American Pediatric Surgical Association, which include the following:
As reconstructive therapy for the compliant pectus deformity, nonoperative compressive orthotic bracing is usually an appropriate first-line therapy as it does not preclude the operative option. For appropriate candidates, orthotic bracing of chest wall deformities can reasonably be expected to prevent worsening of the deformity and often result in a lasting correction of the deformity. Orthotic bracing is often successful in prepubertal children whose chest wall is compliant. Expert opinion suggests that the noncompliant chest wall deformity or significant asymmetry of the pectus carinatum deformity caused by a concomitant excavatum-type deformity may not respond to orthotic bracing.
Thus, in the span of a few decades, conservative management has developed into a widely accepted first-line approach for this congenital deformity. This article summarizes available insight from recent publications as this modality continues to gain popularity in the field of orthotic rehabilitation.
| Overview |
As described, pectus carinatum represents a defect in the growth of the costal cartilage between the ribs and the sternum characterized by an outward protrusion. While this presentation can appear in childhood, it often fails to become apparent until puberty, at which time it can progress in its severity. The efficacy of orthotic management is largely dependent upon its timing, as there is generally a window of opportunity between when the deformity becomes more noticeable and the ossification of the chest wall that comes with continued maturation. If the compressive treatment is initiated during this window, while the chest wall is still pliable, the costal cartilage can be manipulated to a more anatomic position, avoiding the risks of surgery.
A systematic review was published earlier this year, summarizing several observations and considerations related to the conservative management of pectus carinatum. The review drew from 16 publications over a 15-year span, and while the age range of treated individuals varied broadly, it identified an optimal treatment age between 12 and 14 years of age. Patient selection appears to be extremely important to ultimate outcomes but is generally poorly described in clinical trials. A notable exception to this generalization is found in the Dynamic Compression System, discussed in greater detail later in this article, which facilitates the measurement and monitoring of the pressures required to correct the chest deformity and maintain that correction. Within this system, those patients who require corrective pressures deemed excessive are preemptively excluded from conservative management.
Bracing protocols vary but follow a general pattern of near-continuous wear at the initiation of treatment followed by a period of reduced maintenance wear. Initial correction of the pectus generally occurred over a period of four to six months. The subsequent maintenance period reportedly lasted from 14 to 23 months but appeared to be an important consideration in retaining the correction associated with conservative management.
Failure rates ranged widely from “very low” to as high as 43 percent, which were due to noncompliance and loss to follow-up. Complications have typically been reported and are generally below 10 percent, with skin issues being the predominant concern.
The authors of the review summarized their findings as follows:
This treatment modality has been demonstrated to be effective, safe, and reasonably well tolerated but the crucial point to convey here is the high degree of variability in the studies reporting on this technique; not only in the technique protocol itself but factors such as age of patients recruited, length of treatment, outcome measures, and even making some form of appropriate assessment of type and severity of the pectus carinatum, and using that to inform patient selection.
Thus, while conservative management is generally seen as effective, guidance on just how and when it should be implemented is both inconsistent and underinformed in the published evidence.
| Dynamic Compression System |
One well-described approach to conservative management of this population is the Dynamic Compression System. The novelty of the system is found in the associated pressure measuring device, a digital device that allows the treating clinician to measure the average pressure required to initially correct the pectus deformity, thereby documenting its relative flexibility. The recorded pressure, defined as the pressure of correction, serves as a means of assessing candidacy for orthotic management with those patients requiring excessively high corrective pressures recommended for surgery. If the pressure of correction is sufficiently low, bracing is pursued.
The system includes a custom-fitted circumferential aluminum brace consistent in appearance with most pectus carinatum brace designs, including a compression plate that is positioned against the protrusion of the chest wall. The pressure measuring device can be fitted to this compression plate during initial and follow-up fitting appointments to measure the pressure of treatment, or the sustained pressure experienced by the patient while wearing the orthosis. The clinician regularly modifies the brace as necessary to keep this pressure at a tolerable level for the patient.
A fairly recent systematic review of eight clinical trials utilizing the Dynamic Compression System reported that the average ceiling for the pressure of correction that would respond to conservative management was between 7.5 and 10 PSI. Similarly, the average ceiling for the pressure of treatment was reported at 2.5-3.0 PSI. Summarizing data collected from 1,185 patients, the review reported a median age of treatment at 14 years old. The mean study follow-up period was 16 months with 44 percent of patients still under treatment, 29 percent of patients having successfully completed treatment, 6 percent having dropped out, and 21 percent lost to follow-up. Dropout was mainly caused by social discomfort and failure of treatment. Complications were infrequently reported and included mild chest discomfort or tightness and skin lesions. The overall recurrence rate was 2.6 percent. Proponents of this system note both its value in assessing candidacy for conservative management, and objective processes for minimizing excessive corrective pressures, thus reducing the number of patients who might otherwise abandon treatment.
| Bracing After Initial Manual Reduction |
Recognizing that failures in bracing of this population have also resulted from extended treatment periods, Frasure et al. recently reported upon a set of combined modalities in which initial correction through acute manual manipulation was maintained through the use of a stabilizing orthosis. More specifically, using a technique described by the authors as “soft tissue release,” a topical anesthetic and heat were applied prior to a ten-minute manual manipulation of the chest wall cartilage. Sustained pressure was used to flatten the deformity, with an orthosis employed to maintain this correction without applying any additional pressure.
In their retrospective analysis, Frasure et al. reported on 260 patients evaluated for these combined procedures. Of these, 34 presented with deformities that had become too stiff to respond to manual manipulation. These were managed with more traditional bracing with progressive tightening. Two hundred and fifteen patients underwent successful manual reduction of their deformity, with that correction subsequently maintained by the orthosis. At the time of the review, approximately two-thirds of the patients had completed the bracing protocols, with the remaining third continuing to use their devices.
Wearing times were extensive with bracing compliance reported. The average wearing time during the initial phase of brace use was reported at 22.3 hours. Among those who had completed bracing, the average duration of brace use was comparatively short at only 32 weeks (nine months).
| Prescribed Hours of Use |
As suggested earlier, there have been different theories regarding the dosage associated with conservative management of pectus carinatum. Referencing the general trend in the literature advocating near full-time brace wear during the corrective phase of orthosis use, one recent surgical team used a combination of their own data and pooled data from a systematic review to support the counter position of reduced prescribed wear time.6 Motivated by their observation that full-time wear creates social anxiety, discomfort, and skin breakdown, the reporting center advocates only eight to 12 hours of daily use during the initial corrective phase and eight hours per day during the maintenance phase.
Defining success as either full correction or patients progressing successfully at the time of the retrospective review, the center reported a success rate of just over 90 percent, and a compliance rate of 94 percent among the 32 subjects managed with this approach. The authors presented their data alongside the results of a systematic literature review of 15 studies. Here they observed that the centers prescribing full-time brace use during the period of initial correction outnumbered centers prescribing reduced wearing schedules by a ratio of three to one. However, the authors noted that the subjects who were managed with a less intensive prescribed brace usage (less than 12 hours per day) had greater compliance (90 percent), compared to those subjects managed with a more demanding wearing schedule (81 percent). In addition, the authors observed a similar time to correction (roughly seven months) and a similar success rate (about 84 percent) between the two cohorts.
However, these findings are contradicted by a recent randomized controlled trial in which 18 subjects were randomly assigned to either eight-hour or 23-hour wearing schedules. Following three weeks of conservative management, the subjects assigned to the full-time wearing schedule had realized a reduction in their pectus carinatum protrusion that was nearly three times greater than those assigned to the eight-hour wear schedule. The authors observed no differences in adverse events or compliance with the treatment during the three-week observation period, causing them to recommend the greater wearing schedule.
| The Balloon Brace |
A novel approach to the orthotic management of pectus carinatum was recently described in the form of a balloon brace. Placed in a pocket within a non-stretchable binder with Velcro closures, an inflatable balloon is positioned against the anterior chest protrusion. As the balloon is inflated through an external bulb pump, the portion of the chest beneath the balloon is compressed with the variable pressure of the balloon. Air is added until the chest is restored to a flattened contour.
The authors of the report used MRIs to demonstrate the desired depression of the anterior chest wall beneath the balloon. As hoped, the amount of depression correlated well with the amount of air pumped into the balloon. By monitoring oxygen saturation levels, the study authors were able to observe that with the flattening of the chest there was a brief drop, followed by a rapid normalization in oxygen saturation. There were no observed changes in either blood pressure or respiratory rate with the inflation of the balloon.
| Summary |
As bracing continues to grow in popularity as an acceptable means of conservative management of pectus carinatum, a number of recent publications have informed aspects of this care. The Dynamic Compression System suggests an objective method of identifying candidacy for conservative management and ensuring tolerable corrective pressures. Adjunctive manual manipulation has been suggested to expedite the length of treatment with bracing used to maintain rather than create the corrective shape of the chest wall. Questions of bracing dosage have been explored with mixed results and conclusion. Alternatives to traditional rigid bracing structures have also received initial consideration. Collectively, these studies have begun to inform the conservative management of this comparatively emergent patient population.
| Phil Stevens MEd CPO FAAOP is a director with Hanger Clinic’s Department of Clinical and Scientific Affairs. He can be contacted at philmstevens@hotmail.com |
Source THE O&P EDGE
| References |
- Pectus carinatum guideline, American Pediatric Surgical Association, APSA Guideline; 2012.
- Effectiveness of Compressive External Bracing in Patients with Flexible Pectus Carinatum Deformity: A Review, Hunt I, Patel AJ. Thorac Cardiovasc Surg. 2020 Jan;68(1):72-79. doi: 10.1055/s-0039-1687824. Epub 2019 Apr 25. PMID: 31022736.
- Non-surgical treatment of pectus carinatum with the FMF® Dynamic Compressor System, Martinez-Ferro M, Bellia Munzon G, Fraire C, Abdenur C, Chinni E, Strappa B, Ardigo L. J Vis Surg. 2016 Mar 17;2:57. doi: 10.21037/jovs.2016.02.20. Full text
- Measured dynamic compression for pectus carinatum: A systematic review, de Beer SA, Blom YE, Lopez M, de Jong JR. Semin Pediatr Surg. 2018 Jun;27(3):175-182. doi: 10.1053/j.sempedsurg.2018.06.001. Epub 2018 Jun 15.
- External Compressive Bracing With Initial Reduction of Pectus Carinatum: Compliance Is the Key, Fraser S, Harling L, Patel A, Richards T, Hunt I. Ann Thorac Surg. 2020 Feb;109(2):413-419. doi: 10.1016/j.athoracsur.2019.08.026. Epub 2019 Sep 23.
- A less intensive bracing protocol for pectus carinatum, Wahba G, Nasr A, Bettolli M. J Pediatr Surg. 2017 Nov;52(11):1795-1799. doi: 10.1016/j.jpedsurg.2017.01.057. Epub 2017 Jan 31.
- A Comparative Study on Short-Term Effects of Compression Orthosis and Exercises in the Treatment of Pectus Carinatum: A Randomized Controlled Pilot Feasibility Trial, Giray E, Ermerak NO, Bahar-Ozdemir Y, Kalkandelen M, Yuksel M, Gunduz OH, Akyuz G. Eur J Pediatr Surg. 2020 Mar 8. doi: 10.1055/s-0040-1701699. Epub ahead of print.
- Magnetic resonance imaging study of orthotic balloon brace used for the treatment of pectus carinatum, Ewbank C, Idowu O, Chung T, Kim S. Mini-invasive Surg 2018;2:5. http://dx.doi.org/10.20517/2574-1225.2017.51. PDF
| Further reading |
Initial reduction of flexible pectus carinatum with outpatient manipulation as an adjunct to external compressive bracing: technique and early outcomes at 12 weeks, Fraser S, Richards T, Harling L, Patel AJ, Hunt I. J Pediatr Surg. 2020 Jul;55(7):1347-1350. doi: 10.1016/j.jpedsurg.2019.09.024. Epub 2019 Nov 1.
Pectus Carinatum: An Orthotic Approach, Gina M. Retallack CO, David M. Notrica MD and Dawn E. Jaroszewski MD. The O&P Edge April 2013
