Horse riding confirmed as a viable mobility treatment for cerebral palsy
The study shows that functional mobility in children with cerebral palsy can be improved through physical interaction with horses.

Endeavor Therapeutic Horsemanship, Mt. Kisco, NY. Endeavor provides a wide scope of fun filled activities and empowering experiences to participants of all ages and their families. Bill Black photo
Seulhye Kim, Gwangju Institute of Science and Technology GIST, 28 October 2021
Cerebral Palsy (CP) is a common disability among children, characterized by abnormal gait patterns and the inability to maintain posture and balance. While the condition is incurable, physical therapy treatments can go a long way in improving movement and balance.
One such treatment approach is hippotherapy (HPOT), which uses horse riding to improve functional mobility in children with CP. Although supported by scientific studies as an effective treatment approach for (CP), there is, unfortunately, little data concerning how HPOT results in improvement.
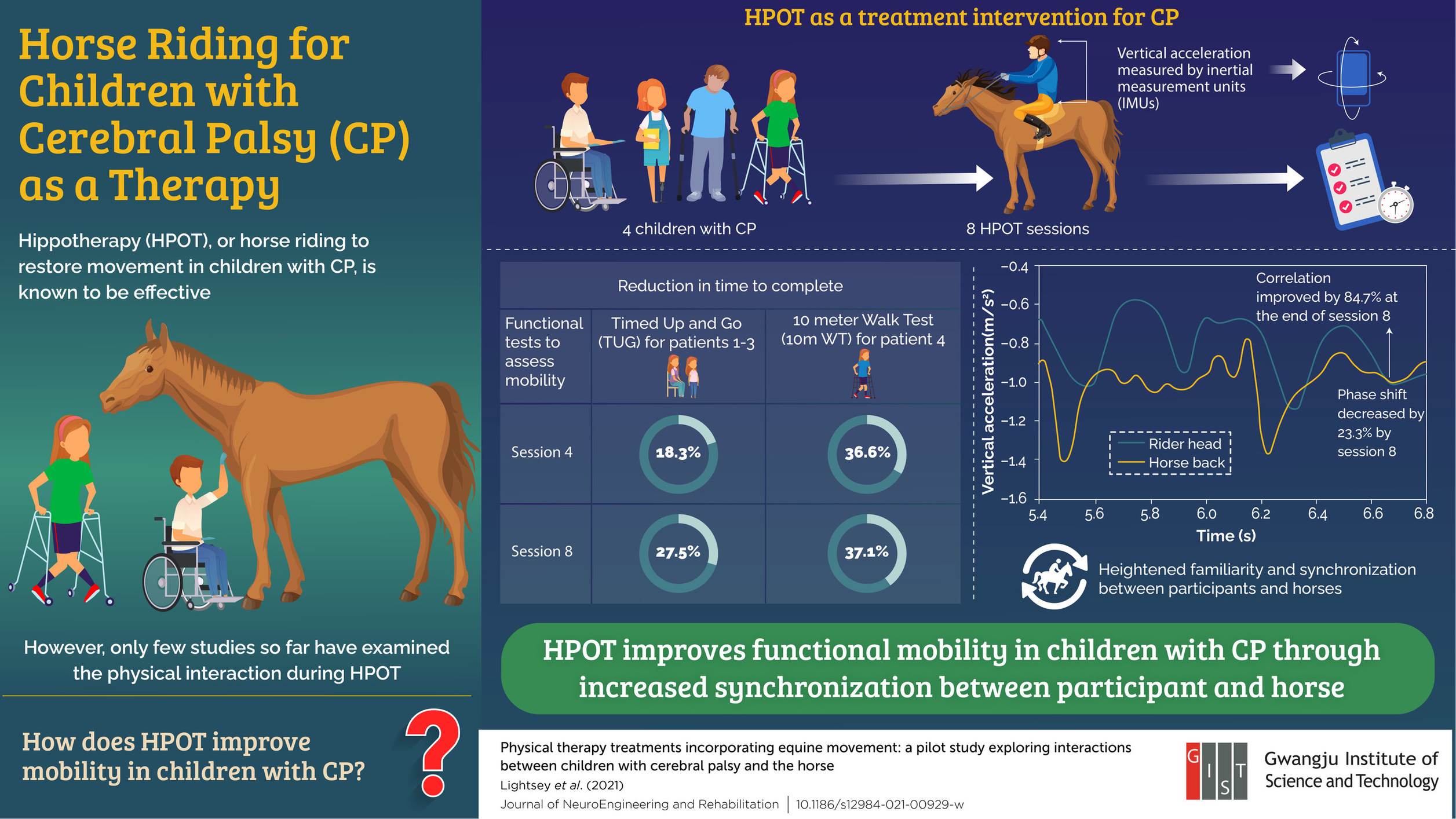
In a recent study, researchers from Gwangju Institute of Science and Technology (GIST) confirm horse riding as a viable mobility treatment for Cerebral Palsy. The study shows that functional mobility in children with cerebral palsy can be improved through physical interaction with horses. Gwangju Institute of Science and Technology (GIST)
Recently, a team of researchers from Korea and the United States addressed this question, investigating physical interaction metrics between horses and children with CP during HPOT. “My original research interests lie in the rehabilitation of people with neurological impairment, specifically gait and balance. However, I did not know about hippotherapy until rather recently in 2016.
After realizing how effective it is in treating children with CP, I was motivated to explore it further,” explains Dr. Pilwon Hur who headed the study from the Gwangju Institute of Science and Technology (GIST) in Korea. This paper was made available online on September 6, 2021, and was published in Volume 18 Issue 132 of the Journal of NeuroEngineering and Rehabilitation.
The research team studied four children with CP over the course of eight physical therapy sessions. They placed sensors on the horses and children to record their movements and track their acceleration and angular velocity. They found that the data from the horses and children began to resemble each other as time progressed, indicating a synchronization between the horse and the rider. They also gave the children mobility tests after each session and observed improvement in their motor skills at the end of the experiment.
“We found that physical interaction between the children with CP and the horses, characterized by the children adapting to the horse’s movement and vice versa, is extremely important for the rehabilitation to be effective,” says Dr. Hur.
Excited by these findings, the team hopes their work will provide a baseline for further research on HPOT. “To the best of my knowledge, ours is the first study to quantify these interactions and relate them to effectiveness,” says Dr. Hur. “Such an understanding would help us optimize physical therapy programs, improving the quality of life for children with CP.”
![]() Source Gwangju Institute of Science and Technology GIST via EurekAlert! AAAS
Source Gwangju Institute of Science and Technology GIST via EurekAlert! AAAS
| References |
Physical therapy treatments incorporating equine movement: a pilot study exploring interactions between children with cerebral palsy and the horse, Priscilla Lightsey, Yonghee Lee, Nancy Krenek & Pilwon Hur. J NeuroEngineering Rehabil 18, 132 (2021). https://doi.org/10.1186/s12984-021-00929-w. Full text, PDF
| Further reading |
Hippotherapy on postural balance in the sitting position of children with cerebral palsy – Longitudinal study, Moraes AG PT, MSc, Copetti F PhD, Ângelo VR BS, Chiavoloni L BS, de David AC PhD. Physiother Theory Pract. 2020 Feb;36(2):259-266. doi: 10.1080/09593985.2018.1484534. Epub 2018 Jun 11.
Do the type of walking surface and the horse speed during hippotherapy modify the dynamics of sitting postural control in children with cerebral palsy? Flores FM, Dagnese F, Copetti F. Clin Biomech (Bristol, Avon). 2019 Dec;70:46-51. doi: 10.1016/j.clinbiomech.2019.07.030. Epub 2019 Jul 25.
Impact of Long-Term Hippotherapy on the Walking Ability of Children With Cerebral Palsy and Quality of Life of Their Caregivers, Mutoh T, Mutoh T, Tsubone H, Takada M, Doumura M, Ihara M, Shimomura H, Taki Y, Ihara M. Front Neurol. 2019 Aug 13;10:834. doi: 10.3389/fneur.2019.00834. Full text
Benefits of hippotherapy in children with cerebral palsy: A narrative review, Martín-Valero R, Vega-Ballón J, Perez-Cabezas V. Eur J Paediatr Neurol. 2018 Nov;22(6):1150-1160. doi: 10.1016/j.ejpn.2018.07.002. Epub 2018 Jul 10.
Effect of Hippotherapy on Motor Proficiency and Function in Children with Cerebral Palsy Who Walk, Champagne D, Corriveau H, Dugas C. Phys Occup Ther Pediatr. 2017 Feb;37(1):51-63. doi: 10.3109/01942638.2015.1129386. Epub 2016 Mar 1.
