Offloading the knee through gait modification
Changing the way people walk can significantly decrease knee external adduction moments, which in turn appears to relieve pain and possibly slow the progression of osteoarthritis. The challenge, however, is finding a gait modification that feels and appears natural to patients.

College of Liberal Arts, Wright State University. Geek with a lens
By Lydia Caldwell BS and Joaquin Barrios PT DPT PhD, Lower Extremity Review August 2011
Osteoarthritis (OA) is a leading cause of functional decline and disability in aging populations, and is associated with staggering economic costs.[1] The joint most often implicated in lower extremity OA is the knee, where major symptoms include pain and stiffness.[2] End-stage knee OA often leads to total knee replacement.[3] Recent epidemiological studies suggest the lifetime risk of developing symptomatic knee OA is close to 50%.[4] This risk is even higher for those who are overweight [3-5] or have a history of knee pathology.[3,4]
Knee OA most often presents in the medial tibiofemoral compartment.[6] This is frequently attributed to an uneven load across the tibiofemoral joint experienced during regular locomotor tasks.[7] It is estimated that the ambulatory load on the medial compartment is approximately 2.5 times greater than the load transferred through the lateral compartment in a normal knee, and approximately 3.3 times greater in individuals with varus alignment.[8] Thus, treatment strategies often target the reduction of these medial loads.
However, direct load measurement is not typically feasible, so knee loads are often assessed indirectly by way of 3D instrumented gait analysis. Indeed, the knee external adduction moment (KEAM) during stance has been found to be highly correlated with medial compartment contact force [9] and is commonly used as a surrogate measure for evaluating joint load.
The KEAM occurs during the stance phase of walking as ground reaction forces are transmitted up the lower limb. From a frontal view, the ground reaction force vector passes medial to the knee joint center, creating a lever arm for knee adduction. The larger this lever arm, the greater the KEAM. This moment typically produces a bimodal waveform with a larger first peak usually occurring between 20% and 30% of stance. Varus alignment is associated with increased adduction moment [10,11,15,24] and has been linked to incident medial knee OA.[12,13] Individuals with medial knee OA demonstrate a higher first peak KEAM than those who are disease free.[14] Furthermore, this first peak has been correlated with both the severity [15] and progression [16] of medial knee OA.
Current rehabilitative therapies for knee OA focus primarily on symptom resolution as a means to functional improvement. Although this goal remains fundamental in the management of medial knee OA, this approach may actually predispose patients to further disease progression in the long term. Gait analysis studies evaluating successful analgesic therapies, such as oral medications and viscosupplementation, have demonstrated that reductions in pain are prospectively related to increases in peak KEAM.[17,18] With time, greater loading of the medial compartment would be expected to accelerate joint deterioration and thus contribute to long-term functional decline. Successful short- and long-term intervention appears to require a shift to a more holistic approach that also targets improved knee biomechanics.
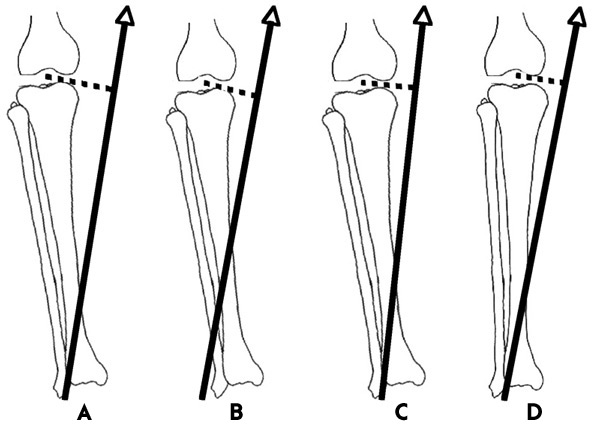
| Figure 1-A. The KAM is predominantly composed of the magnitude of the ground reaction force (arrow and solid line) and its perpendicular distance from the knee joint center of rotation in the frontal plane—the lever arm (dotted line). |
| Figure 1-B. With external rotation of the foot, the position of the center of pressure (origin of the ground reaction force) moves laterally, bringing the GRF closer to the knee joint. |
| Figure 1-C. Leaning the trunk laterally over the stance limb shifts the center of mass laterally. Since the GRF is oriented toward the COM, the vector passes closer to the knee joint; again, a reduced lever arm magnitude and resultant KAM is expected. |
| Figure 1-D. Reduced lever arm and KAM magnitudes can also be accomplished by bringing the knee joint closer to the orientation of the GRF vector. For those with varus malalignment, walking with a more neutrally aligned knee would accomplish this. |
| Michael A. Hunt PT PhD, Lower Extremity Review |
| Gait modification |
Gait modification has become an area of increased research interest due to its potential as a load-reducing intervention. Gait patterns observed to reduce KEAM include increased foot progression angle,[10,19-21] trunk lean,[22,23] medial thrust of the knee,[24] increased hip internal rotation and adduction,[25] and increased weight bearing of the medial aspect of the foot.[26] Gait modification as part of an intervention strategy has several advantages: it can be incorporated into an existing therapeutic program without additional cost, does not require orthotics or bracing, and patients can engage in gait modification on their own after they receive appropriate training.
A longitudinal study by Wang et al revealed a link between preoperative KEAM and rates of clinical success following high tibial osteotomy to reduce medial knee load.[10] More than five years postoperatively, patients with lower preoperative KEAM were 37% more likely to maintain their valgus realignment than those with higher preoperative KEAM. Gait analysis indicated that peak inversion moment at the ankle, which is related to the rotational position of the foot, was significantly greater in those with higher KEAM. This relationship suggests that toeing-out may be a valuable mechanism for reducing knee load. This relationship is also consistent with a study investigating foot progression angle in healthy participants that demonstrated that those who walk with a large toe-out angle had significantly lower peaks in KEAM during the late stance phase of walking than those who walked with less toe-out of the foot.[19] A study investigating the use of increased foot progression angle in participants with mild to moderate medial compartment knee OA showed that increasing foot progression angle by 15° reduced the second peak of the KEAM by 40%.[21]
Relatively little is known regarding the clinical implication of reducing the second peak of the KEAM; however, support for such a strategy can be found in a study that documented a decreased likelihood of disease progression with increased foot progression angle. Toe-out angle at baseline was greater in individuals who did not demonstrate radiographic progression of medial knee OA at an 18-month follow up than in those whose OA did progress.[20] The observed reduction in adduction moment may be attributed to a lateral shift in the center of pressure, which theoretically causes the ground reaction force vector to pass closer to the knee, thereby reducing the aforementioned lever arm.[20]
| Trunk lean |
Whereas increased foot progression angle appears to significantly reduce loading during late stance, trunk lean has demonstrated reductions throughout the entire stance phase. This gait pattern is characterized by increasing lateral sway of the trunk over the stance limb. In a study of 19 healthy participants, increasing mediolateral trunk sway by an average of 10° led to a 65% reduction in the KEAM.[22] This reduction in medial loading occurred without significant changes to secondary gait mechanics affecting the lower extremity, such as lateral ground reaction force and axial loading rates.[22] In addition, the magnitude of KEAM reduction suggests that even smaller alterations in trunk kinematics could still provide significant reductions in medial joint loading.
In contrast to the study by Mündermann and colleagues in which participants walked with a self-selected amount of trunk lean,[22] Hunt et al investigated the use of feedback-driven ipsilateral trunk lean to reduce the KEAM as well as to assess associated levels of task difficulty and discomfort.[23] Participants received a single session of kinematic feedback to walk with trunk lean conditions of 4°, 8°, and 12°. Each condition led to reductions in KEAM, with greater lean resulting in larger reductions. These three conditions led to average reductions of 7%, 21%, and 25%, respectively.[23]
However, all participants in this study reported some difficulty in implementing the desired walking pattern, and three of the nine participants reported mild discomfort. The difference in joint loading between trunk lean of 8° and 12° was statistically insignificant; however, the larger degree of lean was associated with greater task difficulty. Thus, trunk lean of 8° was determined to be the most advantageous of the conditions.[23]

High Speed 120FPS Video Gait Analysis. East Coast Podiatry Clinic
| Keeping up appearances |
One critique of gait modifications such as increased foot progression angle and ipsilateral trunk lean is that they appear different than natural gait. Fregly et al set out to develop a “normal looking” gait pattern that was capable of reducing both peaks of the KEAM.[24] In a 2007 single-subject study, inverse dynamic optimization was used to predict gait modifications that could reduce KEAM without altering foot path, trunk orientation, or arm motion.[24]
The optimization resulted in a model known as “medial-thrust” gait. The pattern is characterized by increased hip, knee, and ankle flexion and concurrent medial thrust of the knee. After nine months of self-retraining by the patient, this gait pattern resulted in KEAM reductions of up to 55%. Even more significant is that KEAM reductions of up to 39% were maintained even when the patient attempted to walk using his former gait pattern.[24] The reduction is attributed to a more lateral trajectory of the ground reaction force vector resulting in a shorter lever arm.
A 2009 single-subject study in which investigators collected in vivo contact force data from the participant with a force-measuring knee replacement confirmed the ability of the medial-thrust gait pattern to reduce contact forces in the knee.[27] The medial-thrust gait pattern resulted in a 16% reduction in medial contact force over stance phase when compared with the participant’s natural gait.
A 2009 single-subject study in which investigators collected in vivo contact force data from the participant with a force-measuring knee replacement confirmed the ability of the medial-thrust gait pattern to reduce contact forces in the knee.[27] The medial-thrust gait pattern resulted in a 16% reduction in medial contact force over stance phase when compared with the participant’s natural gait.
Participants reported that performance of the prescribed modification required less effort and became more natural feeling over the course of the training period. The modified gait pattern was easily reproduced at a one-month follow-up session at which participants showed maintenance of the 20% KEAM reduction. However, no changes were seen in participants’ natural walking pattern when compared with baseline kinetics, implying that the altered pattern still needed to be volitionally engaged.
Another study effectively altered the KEAM by increasing weight bearing to the medial side of the foot.[26] Participants were instructed to minimally load the lateral side of the foot in order to shift pressure medially. Implementation of this gait pattern under verbal feedback from investigators led to an 8% decrease in KEAM relative to baseline. When active feedback was employed using a pressure-activated pager, the result was a 14% reduction in KEAM compared with natural-gait trials. The significant improvement made with the use of active feedback suggests that this method may prove beneficial in the instruction and internalization of novel gait patterns. Techniques aimed at optimizing patients’ learning process need to be developed for successful implementation of gait modification.
Shull et al used a haptic feedback system to train nine healthy participants in a multiparameter data-driven gait model.[28] A skin stretch device on individuals’ lower back provided feedback on trunk sway, while vibration motors on the knee and foot responded to the lateral tibia and foot progression angles. All three parameters were altered simultaneously. Final gait parameter changes were specific to each individual participant based on the influence of each of the parameters on the KEAM. Gait retraining occurred during a single session and resulted in KEAM reductions of 29% to 48% when compared with participants’ natural gait.
It is clear from the current literature that gait modification strategies are capable of significantly reducing the KEAM. Importantly, Miyazaki et al [16] demonstrated that higher magnitudes of peak KEAM dramatically increase the risk of medial knee OA progression. Thus, the potential for gait modification to slow the progression of medial knee OA is at least plausible and worth exploring, given that no conservative intervention has been found to slow knee OA. Decelerating disease progression could reduce the number of patients requiring total knee replacements and other invasive and costly procedures related to end-stage OA, or at least significantly delay the need for such procedures.

| Challenges |
Compliance is the predominant barrier foreseen in implementation of gait modification. As with any therapy, adherence to an intervention is often enhanced when patients can appreciate changes in symptoms. Thus, a major question is whether or not gait modification strategies can appreciably affect pain or other symptoms. In a study of more than 100 patients with medial knee OA, larger adduction moments were associated with more severe pain.[16] A study investigating the KEAM between symptomatic and asymptomatic knee OA patients of the same radiographic progression, reported that those with symptomatic knee OA had a peak adduction moment 19% greater than those who were symptom free.[29] This seems to suggest that reducing the KEAM—as has been observed in the performance of various gait modifications—may lead to symptom reduction of medial knee OA.
Perhaps one of the most common criticisms against load modulation strategies in patients with knee OA is based on studies that fail to find relationships between pain and KEAM. Indeed, Maly and colleagues found no relationship between pain and KEAM in 53 patients with OA.[30] However, the pain-loading relationship is not straightforward and may be confounded by numerous factors, such as disease severity, pain chronicity, joint laxity, climate, and hormonal factors, among others. Despite this, our current understanding of the pain-loading relationship is largely based on cross-sectional analyses instead of studies that experimentally manipulate the KEAM as an independent variable and track pain as a dependent variable.
Second, it is the belief of the authors that load modulation is primarily aimed at slowing disease progression over months and years, and that any associated clinical changes are typically modest on an acute level. Other clinical interventions (strengthening, stretching, modalities such as therapeutic ultrasound, viscosupplementation, etc.) need to be concomitantly delivered to optimally reduce pain and enhance functional status on an acute basis.

NIMBLE SCIENCE. The Gait Lab inside Drexel’s new College of Nursing and Health Professions facility is equipped with cameras and wearable markers to help researchers study running movements and foot strike patterns.
| Looking ahead |
However, just recently, a single-patient study was published documenting gait modification and pain response to walking trials that included increased foot progression angle and lateral trunk lean.[31] Degree of modification was self-selected and level of pain was expressed using a rating scale in which zero meant no pain and 10 indicated maximal pain. In a patient with medial knee OA, natural gait resulted in a pain response of 4/10. The same level of pain was expressed immediately following a 10° increase in foot progression angle, but decreased to 3/10 with 6° of lateral trunk lean. The 10° increase in foot progression angle resulted in a 6% decrease in peak KEAM while 6° of trunk lean reduced the peak KEAM by 53%. These results are promising in that increased trunk lean was capable of eliciting an immediate and appreciable reduction in pain. Further exposure and practice of the new gait pattern could result in even further reductions to load-related pain.
Very few gait modification studies have involved patients with symptomatic medial knee OA. Further research is needed to elucidate the potential role of gait modification in the management of knee OA. Based on our current understanding of the deleterious effects of high medial joint loading, we must explore options that can reduce loading with the global aim of slowing disease progression. Intervention strategies that incorporate gait modification in conjunction with symptom resolution and functional enhancement may prove beneficial for both the short and long term. For clinicians to successfully treat the cause and not merely the symptoms of medial knee OA, load-reducing strategies such as gait modification must be explored.
| Lydia Caldwell BS, is currently pursuing a master’s degree in exercise science from the University of Dayton in Ohio. Joaquin Barrios PT DPT PhD, is an assistant professor in the Department of Health Science at the University of Dayton and directs the Motion Analysis Laboratory housed within the Doctor of Physical Therapy Program. |
Source Lower Extremity Review
| References |
- The economic burden of osteoarthritis, Bitton R. Am J Manag Care. 2009 Sep;15(8 Suppl):S230-5. Full text
- Incidence of symptomatic hand, hip, and knee osteoarthritis among patients in a health maintenance organization, Oliveria SA, Felson DT, Reed JI, Cirillo PA, Walker AM. Arthritis Rheum. 1995 Aug;38(8):1134-41.
- Osteoarthritis: new insights. Part 1: the disease and its risk factors, Felson DT, Lawrence RC, Dieppe PA, Hirsch R, Helmick CG, Jordan JM, Kington RS, Lane NE, Nevitt MC, Zhang Y, Sowers M, McAlindon T, Spector TD, Poole AR, Yanovski SZ, Ateshian G, Sharma L, Buckwalter JA, Brandt KD, Fries JF. Ann Intern Med. 2000 Oct 17;133(8):635-46. Review. Full text
- Lifetime risk of symptomatic knee osteoarthritis, Murphy L, Schwartz TA, Helmick CG, Renner JB, Tudor G, Koch G, Dragomir A, Kalsbeek WD, Luta G, Jordan JM. Arthritis Rheum. 2008 Sep 15;59(9):1207-13. doi: 10.1002/art.24021. Full text
- Knee osteoarthritis and obesity, Coggon D, Reading I, Croft P, McLaren M, Barrett D, Cooper C. Int J Obes Relat Metab Disord. 2001 May;25(5):622-7.
- Osteoarthrosis of the knee. A radiographic investigation, Ahlbäck S. Acta Radiol Diagn (Stockh). 1968:Suppl 277:7-72. No abstract available.
- In vivo medial and lateral tibial loads during dynamic and high flexion activities, Zhao D, Banks SA, D’Lima DD, Colwell CW Jr, Fregly BJ. J Orthop Res. 2007 May;25(5):593-602. PDF
- Interaction between active and passive knee stabilizers during level walking, Schipplein OD, Andriacchi TP. J Orthop Res. 1991 Jan;9(1):113-9.
- Correlation between the knee adduction torque and medial contact force for a variety of gait patterns, Zhao D, Banks SA, Mitchell KH, D’Lima DD, Colwell CW Jr, Fregly BJ. J Orthop Res. 2007 Jun;25(6):789-97. PDF
- The influence of walking mechanics and time on the results of proximal tibial osteotomy, Wang JW, Kuo KN, Andriacchi TP, Galante JO. J Bone Joint Surg Am. 1990 Jul;72(6):905-9.
- Lower extremity walking mechanics of young individuals with asymptomatic varus knee alignment, Barrios JA, Davis IS, Higginson JS, Royer TD. J Orthop Res. 2009 Nov;27(11):1414-9. doi: 10.1002/jor.20904. PDF
- Association between valgus and varus alignment and the development and progression of radiographic osteoarthritis of the knee, Brouwer GM, van Tol AW, Bergink AP, Belo JN, Bernsen RM, Reijman M, Pols HA, Bierma-Zeinstra SM. Arthritis Rheum. 2007 Apr;56(4):1204-11. PDF
- The role of knee alignment in disease progression and functional decline in knee osteoarthritis, Sharma L, Song J, Felson DT, Cahue S, Shamiyeh E, Dunlop DD. JAMA. 2001 Jul 11;286(2):188-95. Erratum in: JAMA 2001 Aug 15;286(7):792.
- Increased knee joint loads during walking are present in subjects with knee osteoarthritis, Baliunas AJ, Hurwitz DE, Ryals AB, Karrar A, Case JP, Block JA, Andriacchi TP. Osteoarthritis Cartilage. 2002 Jul;10(7):5. PDF
- Knee adduction moment, serum hyaluronan level, and disease severity in medial tibiofemoral osteoarthritis, Sharma L, Hurwitz DE, Thonar EJ, Sum JA, Lenz ME, Dunlop DD, Schnitzer TJ, Kirwan-Mellis G, Andriacchi TP. Arthritis Rheum. 1998 Jul;41(7):1233-40.
- Dynamic load at baseline can predict radiographic disease progression in medial compartment knee osteoarthritis, Miyazaki T, Wada M, Kawahara H, Sato M, Baba H, Shimada S. Ann Rheum Dis. 2002 Jul;61(7):617-22. Full text
- Knee pain and joint loading in subjects with osteoarthritis of the knee, Hurwitz DE, Ryals AR, Block JA, Sharma L, Schnitzer TJ, Andriacchi TP. J Orthop Res. 2000 Jul;18(4):572-9.
- Medial knee joint loading increases in those who respond to hyaluronan injection for medial knee osteoarthritis, Briem K, Axe MJ, Snyder-Mackler L. J Orthop Res. 2009 Nov;27(11):1420-5. doi: 10.1002/jor.20899. PDF
- Lower limb alignment and foot angle are related to stance phase knee adduction in normal subjects: a critical analysis of the reliability of gait analysis data, Andrews M, Noyes FR, Hewett TE, Andriacchi TP. J Orthop Res. 1996 Mar;14(2):289-95.
- The relationship between toe-out angle during gait and progression of medial tibiofemoral osteoarthritis, Chang A, Hurwitz D, Dunlop D, Song J, Cahue S, Hayes K, Sharma L. Ann Rheum Dis. 2007 Oct;66(10):1271-5. Epub 2007 Jan 31. Full text
- The influence of foot progression angle on the knee adduction moment during walking and stair climbing in pain free individuals with knee osteoarthritis, Guo M, Axe MJ, Manal K. Gait Posture. 2007 Sep;26(3):436-41. Epub 2006 Nov 28.
- Implications of increased medio-lateral trunk sway for ambulatory mechanics, Mündermann A, Asay JL, Mündermann L, Andriacchi TP. J Biomech. 2008;41(1):165-70. Epub 2007 Aug 3.
- Feasibility of a gait retraining strategy for reducing knee joint loading: increased trunk lean guided by real-time biofeedback, Hunt MA, Simic M, Hinman RS, Bennell KL, Wrigley TV. J Biomech. 2011 Mar 15;44(5):943-7. doi: 10.1016/j.jbiomech.2010.11.027. Epub 2010 Dec 7.
- Design of patient-specific gait modifications for knee osteoarthritis rehabilitation, Fregly BJ, Reinbolt JA, Rooney KL, Mitchell KH, Chmielewski TL. IEEE Trans Biomed Eng. 2007 Sep;54(9):1687-95. Erratum in: IEEE Trans Biomed Eng. 2007 Oct;54(10):1905. Full text
- Gait retraining to reduce the knee adduction moment through real-time visual feedback of dynamic knee alignment, Barrios JA, Crossley KM, Davis IS. J Biomech. 2010 Aug 10;43(11):2208-13. doi: 10.1016/j.jbiomech.2010.03.040. Epub 2010 May 8. Full text
- Gait modification via verbal instruction and an active feedback system to reduce peak knee adduction moment, Dowling AV, Fisher DS, Andriacchi TP. J Biomech Eng. 2010 Jul;132(7):071007. doi: 10.1115/1.4001584.
- Effective gait patterns for offloading the medial compartment of the knee, Fregly BJ, D’Lima DD, Colwell CW Jr. J Orthop Res. 2009 Aug;27(8):1016-21. doi: 10.1002/jor.20843. Full text
- Training multi-parameter gaits to reduce the knee adduction moment with data-driven models and haptic feedback, Shull PB, Lurie KL, Cutkosky MR, Besier TF. J Biomech. 2011 May 17;44(8):1605-9. doi: 10.1016/j.jbiomech.2011.03.016. Epub 2011 Apr 2.
- Relationship between pain and medial knee joint loading in mild radiographic knee osteoarthritis, Thorp LE, Sumner DR, Wimmer MA, Block JA. Arthritis Rheum. 2007 Oct 15;57(7):1254-60. PDF
- Mechanical factors relate to pain in knee osteoarthritis, Maly MR, Costigan PA, Olney SJ. Clin Biomech (Bristol, Avon). 2008 Jul;23(6):796-805. doi: 10.1016/j.clinbiomech.2008.01.014. Epub 2008 Mar 17.
- Varus thrust in medial knee osteoarthritis: quantification and effects of different gait-related interventions using a single case study, Hunt MA, Schache AG, Hinman RS, Crossley KM. Arthritis Care Res (Hoboken). 2011 Feb;63(2):293-7. doi: 10.1002/acr.20341. No abstract available. Full text
Also see
Knee OA: The evidence for gait modification Lower Extremity Review
Gait Keepers Drexel University

