Part 2: When a knee replacement specialist needs his own new knee
A noted surgeon gains insight into managing postop pain—his own.
In part 1 of his account of his knee replacement surgery, knee replacement specialist Ira H. Kirschenbaum MD, chairman of the Department of Orthopedics at Bronx-Lebanon Hospital Center, Bronx, New York, described his experience as a patient up to and including his procedure.
Ira H. Kirschenbaum MD, Medscape Orthopedics October 05, 2016
Here, in part 2, Dr Kirschenbaum discusses postoperative pain management, including the effectiveness of the multimodal pain management techniques his surgeon prescribed, his need for opioid medication; and the physical aspects of his recovery.
| Tired but Good |
| August 25, 2016 |
This is postoperative day 3. This has been a good day so far. My pain ranges from a best of 1 to a worst of 3 out of 10 on a visual pain scale. I haven’t taken anything but Tylenol® and Aleve® all day. I’m able to stand up pretty nicely for a patient who has had his left knee replaced. I’m a bit surprised, actually. I have always thought that my patients would have been in worse shape by this time in terms of pain, but we’ve been pretty aggressive with the multimodal pain medicines and ice. It’s working.
Last night was the last time I took any narcotics. I only took 10 mg of oxycodone at about 9 PM. I ended up waking up at 2:30 AM with a little bit of discomfort that was well controlled with two Tylenol. That’s my pain story.
My knee function is quite good. I’m walking a bit better. I have a knee exercise that I’ll be doing more of today. I do get tired a lot sooner than I would have expected. After walking around a lot this morning, I found myself very tired by 10:30 AM. I think a lot of my body energy is being directed toward my knee to heal it, so the rest of my body becomes correspondingly tired.
I’m not getting dizzy or having any imbalance while walking, but I am aware that when I’m starting to get a little tired, I need to sit or lay down and rest. I took a nap this morning for about an hour and a half, something I don’t usually do. The key is to be sensitized to my degree of tiredness, keep the fluids going, and keep the multimodal pain medications going. Other than that, it’s been a good day.
| The Real World |
| August 26, 2016 |
Woke up on this fourth day after surgery feeling remarkably well. Some generalized soreness, but I was able to move my knee to 103 degrees. How do I know? Measuring a joint is done with a goniometer. And yes, there is a smartphone app for that.
Today I advanced to a cane. I had been using a walker. A cane felt more natural, and since I did some quadriceps exercises yesterday, my quadriceps strength is improving. As I was instructed in my physical therapy session before the operation, I gripped the cane in my right hand, the hand opposite my new knee, and carefully started walking. I was pumped. I managed to get my clothes on (regular clothes, by the way), climbed into a car (as a passenger), and went out into the real world.
Getting into the car was not hard. I decided to sit in the back seat. I went over to my friend’s business office and hung out for a couple of hours. Had lunch, worked on the computer, made some phone calls. As I mentioned yesterday, after major surgery, this kind of mental effort tires you out. My advice to patients is this: Whatever discomfort, pain, or fear you experience in the first few days, have faith that it will subside in a short while.
| Thinking About Pain |
| August 27, 2016 |
It is now Saturday, the fifth day after my surgery. I am well past the time when most patients and surgeons conventionally feel that patients experience the most pain. I now have minor discomfort only.
In my experience as a surgeon, total knee replacement is an operation in which we traditionally use quite a lot of opioids. Yet my opioid use has been minimal. A lot of it has to do with the adoption of modern multimodal pain techniques by my surgeon, which more and more surgeons are using. These techniques include intravenous acetaminophen (Ofirmev®) on a particular protocol; injections of liposomal bupivacaine (Exparel®) in the operating room mixed with standard bupivacaine; ice therapy; early mobilization; oral Tylenol around the clock; and nonsteroidal anti-inflammatory drugs (NSAIDs) both preop and immediately postop.
I’ve been on this regimen since last Monday, when I had my procedure. Since then, I’ve taken oxycodone in 10-mg doses for a total of 30 mg over 4 days. I have taken no other opioids. Partly this is attributable to the success of the multimodal pain techniques. But I also attribute it to the expectations and trust I had that the pain would not be as great as what others who have had this surgery suggested it would be.
My experience raises a number of questions. For example, when did I experience the most pain, how bad was it, and how did I manage it?
I had the surgery on a Monday. I probably had the most pain from Tuesday afternoon to late Tuesday evening. This was a time when I think the standard bupivacaine was wearing off and the liposomal bupivacaine was kicking in—what is called a “bridging” time. The pain drifted to about 4 or 5 out of 10 on the pain scale—never more than that—and then by Wednesday morning the pain diminished to about a 3 as the liposomal bupivacaine started working at its full impact. So the pain was quite manageable using the multimodal techniques.
At many hospitals, knee replacement patients receive two Percocets (two 10-mg tablets of acetaminophen/oxycodone) every 4-6 hours. Some hospitals give 30 mg of oxycodone twice a day in addition to that. My experience belies this approach. We have been stuck in a rut in the way we order opioids. In my case, I was able to use significantly lower amounts of pain medicine. I think the narcotics we give the patients to control pain need to be at a much lower dosage, and they need to be given over greater time periods. We also need to adopt a multilevel pain regimen that includes intravenous acetaminophen and liposomal bupivacaine, which reduce pain in the knee for 24-72 hours.
I have used standard bupivacaine and, separately, standard bupivacaine with liposomal bupivacaine in my practice, and I have seen an absolute improvement in patients’ pain on the second and third days from the use of liposomal bupivacaine. Whether this decreased the length of stay is hard to say, because we have a very short length of stay at my hospital (the average is around 2 days). I had my procedure as an outpatient, so length of stay was not my endpoint. Instead, my endpoints were patient satisfaction and patient satisfaction with pain relief, which was significantly better with the liposomal bupivacaine.
I felt the bupivacaine wear off at about 11 PM on Monday, the day of my surgery. I had a short period of discomfort until the liposomal bupivacaine kicked in, which it definitely did, because I had significant pain relief most of Tuesday, when I did a fair amount of exercise. Tuesday night my knee was sore, but the liposomal bupivacaine, continued to work. On Wednesday I had pain of between 1 and 3 on the pain scale. That could only really be explained by the use of bupivacaine/liposomal bupivacaine, which allowed me to severely limit my use of opioids in the first couple of days. It also helped me prevent any dependency I might have developed, which might have caused me to reach for a pill for the pain.
| No Place Like Home |
| August 31, 2016 |
Today is Wednesday, a 9 days after my surgery. Two days ago, I traveled from Seattle, where the surgery was performed, back to New York, where I live. I chose to have my knee done, as an outpatient, by a close friend and colleague in Seattle. Aside from the inherent trust I had in my surgeon, I also am a firm believer in his enhanced recovery protocols. I use these protocols in my own practice.
But no matter how modern these techniques are, total knee replacement is still a major operation. Regaining the ability to be safely mobile is a gradual process. I was still quite concerned about navigating through the airport, spending hours on a plane, and then getting back to my house.
In joint replacement surgery, surgeons are concerned about the development of blood clots in the legs in the first few weeks postop. These clots can travel from the legs to a lung, causing serious health problems. Spending 5-6 hours in the air while possibly immobile needs to be mitigated. I had early mobility the first day after my surgery, sequential compression devices for over 12 hours a day on my legs, and chemical prophylaxis with warfarin (Coumadin®) for 3 days, followed by enoxaparin (Lovenox®) injections (self-injected) each day.
These therapies were continued in flight. Enoxaparin aggressively thins the blood. Sitting in my seat on the plane, fully anticoagulated and with my leg pumps, and getting up every half-hour to stay mobile, gave me peace of mind.
| The Caregiver’s Essential Role |
| September 5, 2016 |
I don’t believe that anyone can go through a knee replacement operation alone. You either need a mobile and dedicated caregiver 24 hours a day for a solid 2 weeks or you need to go to some type of rehab hospital.
In recent years, there has been talk about joint replacement patients not needing to go to rehab facilities and instead recuperating at home. I suspect that this chatter has been perpetrated by government and insurance company administrators, and not by anyone who cares about the safety and satisfaction of patients, because patients who live alone or have limited caregivers at home cannot go home immediately after surgery.
Here is a partial list of what a caregiver does:
- Makes sure that all of the prescriptions are available and within the patient’s reach;
- Ensures that the patient has access to food;
- Helps position the patient on a chair or bed at times when the patient feels tired or dizzy;
- Observes the patient to ensure that he or she is walking safely;
- Helps the patient in the bathroom negotiate from the toilet to the shower;
- Helps the patient change ice packs;
- Fetches pain medications for the patient in the middle of the night as needed;
- Assists in transferring the patient from bed to chair to other rooms; and
- Helps in the communication with the patient’s doctor in times of need.
You need a person in the house full-time. A home health aide who is there for 4 hours a day, while helpful, is not enough. You need basic, non-medical help around the clock. If you don’t have that, then while you may not need to go to the most intense rehab facility in the world, you will require a 5- to 10-day stay at a basic skilled nursing facility that understands the joint replacement healing process. They will need to get you up and mobile 6-8 times a day; apply cooling therapy for your comfort, as needed; provide pain medications (if needed); and conduct formal physical therapy at least twice a day.
| A View Down the Line |
| September 22, 2016 |
I am now at 4 weeks post-surgery. The journey of healing is really amazing. It’s not a linear experience. There are quite a few ups and downs; during the ups, everything feels great; during the downs, even I, as a surgeon, was getting worried. These vacillations primarily relate to function, motion, general vitality, and pain.
Let me start with how I am at 4 weeks:
- I am walking well with no pain.
- I can walk up steps in a normal manner, barely needing to use the railing.
- Walking down steps is still difficult; I use the railing and place my hand on a wall on the other side for support. Sometimes I walk down with two feet on one step at a time.
- I can walk for about a quarter-mile around my neighborhood. I have not needed a cane since the end of week 1.
- My leg is fully straight and I can bend my knee to a 121-degree angle. I started driving this week without problems.
I’ve been going to physical therapy three times a week for 90-minute sessions, which include moist heat, manual massage, quad sets (a number of different exercises), extension and flexion stretches, stationary bicycle, hamstring stretches, and a compressive cooling device.
When I am home, I use my stationary bicycle and continue the exercises I learned in preop and postop physical therapy. I heat up my knee a couple of times a day and ice it down about three times a day.
I start my day with 325 mg of aspirin, 660 mg of Aleve, and 650 mg of Tylenol. I take no more Tylenol or Aleve for the rest of the day. The aspirin is for anticoagulation, so I take another tablet at night.
I have not felt the need for any further opioid medication.
I think the keys to opioid reduction are:
- Preoperative patient education—really getting the patient to know what to expect regarding pain is critical.
- Preoperative caregiver education—almost as important as the first point.
- The use of multimodal pain techniques: IV acetaminophen (Ofirmev®); injections during surgery that include liposomal bupivacaine (Exparel®), which extend the pain relief for 2-3 days; NSAIDs (I used Aleve but some people use Celebrex®; it depends on what your stomach can tolerate); Tylenol 650 mg every 4 hours; surgical techniques that protect from excess tissue damage; early activity, including range-of-motion exercises; and frequent ice packs/cooling of the knee.
I will be returning to work the first week of October. Since I am the chairman of orthopedics at my hospital, my entire staff is going to be pleased, mainly because the ceaseless flow of emails I am sending them from home will stop—or at least abate.
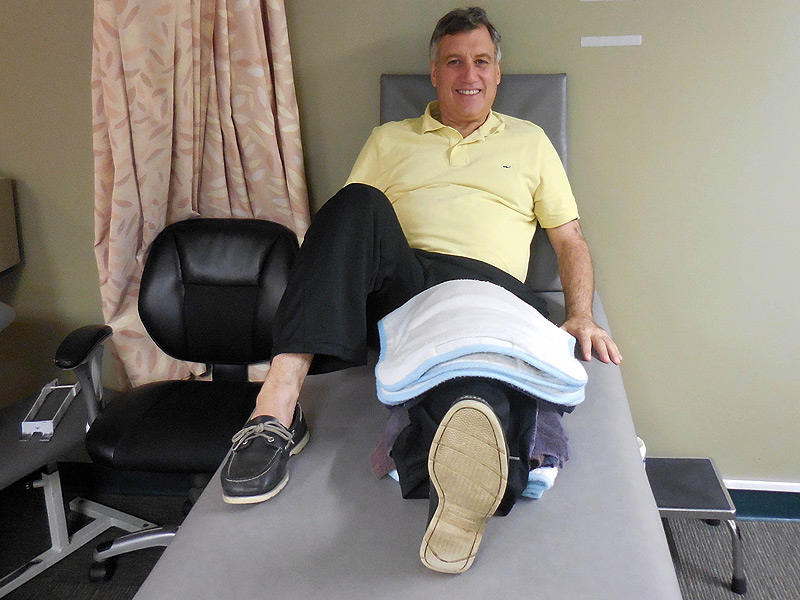
| Here is a cool knee exerciser I am using. Ira H. Kirschenbaum MD, My Knee Your Knee |
Source Medscape
Also see
How much time will I have to be off work for knee replacement surgery? Bone Smart
Your Risk of Infection After Knee Replacement Depends on Your Hospital Consumer Reports
